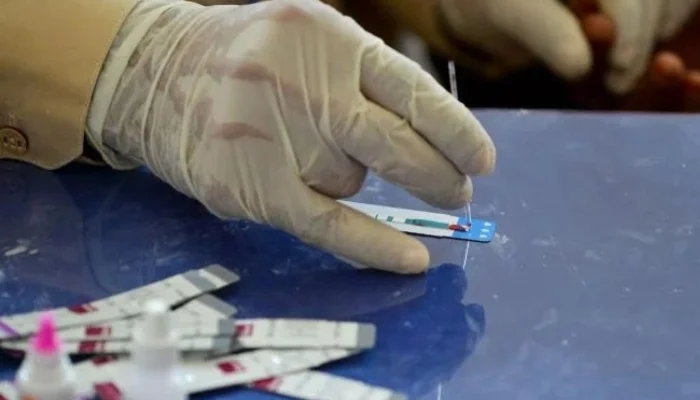
A major public health concern has emerged in Pakistan after lawmakers were informed that nearly 20,000 HIV patients who began treatment have become untraceable. The issue was highlighted during a meeting of the National Assembly Standing Committee, where officials expressed concern over gaps in patient follow-up and long-term care.
Health authorities described the situation as serious and urgent. They admitted that maintaining contact with patients after treatment begins remains a major challenge. As a result, many individuals discontinue therapy, increasing the risk of disease spread and complications. Lawmakers stressed that a coordinated national strategy is needed to address these gaps effectively.
Rising HIV Cases and Gaps in Detection
Officials from the health ministry revealed that an estimated 369,000 people are currently living with HIV in Pakistan. However, only about 84,000 cases are officially registered. This large gap highlights major issues in detection, reporting, and awareness.
In addition, around 14,000 new HIV cases were reported in 2025 alone. This increase has raised concerns about the effectiveness of current prevention efforts. Although testing has improved significantly, experts warn that detection alone does not indicate control over the disease.
Screening numbers have increased sharply in recent years. Testing rose from 37,000 cases in 2020 to over 374,000 in 2025. Despite this progress, lawmakers emphasized that the real goal should be reducing new infections, not just increasing the number of tests conducted.
Local Outbreaks Expose Weak Health Practices
Committee members pointed to repeated outbreaks in regions such as Taunsa, Kot Momin, and parts of South Punjab. These outbreaks highlight weaknesses in infection control measures and unsafe medical practices.
During the briefing, officials also discussed an outbreak in Karachi’s Walika area. Investigations linked the spread to the use of certain syringes that had not been effectively regulated. Authorities now plan to phase out reusable syringes and introduce stricter controls on medical equipment.
Lawmakers questioned why banned syringes are still available in markets. They raised concerns about weak enforcement of existing regulations. They also pointed to poor oversight of blood banks and unsafe clinical practices as contributing factors.
Social Stigma and Patient Dropout Add to Crisis
Another major issue discussed was the high number of patients who stop treatment after diagnosis. Social stigma around HIV continues to discourage people from seeking care or continuing therapy. This results in many patients becoming untraceable after initial treatment begins.
Officials acknowledged that counseling and patient support systems are not strong enough. Without proper follow-up, patients often drop out of treatment programs. This not only affects their health but also increases the risk of further transmission.
Lawmakers stressed the need for nationwide awareness campaigns to reduce stigma and encourage testing and treatment. They also called for better systems to track and support patients throughout their treatment journey.
Cross-Border Risks and Need for Immediate Action
The committee also discussed health risks linked to cross-border movement. Officials noted that individuals returning from other countries are not always properly screened. To address this, the government is developing a system to link travel data with health monitoring. This will help ensure screening before re-entry into the country.
While the health ministry is preparing a comprehensive plan to tackle the HIV crisis, lawmakers demanded immediate action. They called for the introduction of auto-disable syringes, strict enforcement against unsafe medical practices, and a clear timeline for implementation.
The committee emphasized that the situation requires urgent and coordinated efforts. Without immediate intervention, the spread of HIV could become more difficult to control in the coming years.